
Final alternate jurors chosen in Trump trial as opening statements near
The final five alternate jurors in former President Donald Trump's New York criminal trial were selected on Friday.
Watch CBS News

The final five alternate jurors in former President Donald Trump's New York criminal trial were selected on Friday.

A person self-immolated at a park across from the courthouse where former President Donald Trump's New York criminal trial is taking place.

Two U.S. officials tell CBS News an Israeli missile has hit Iran in apparent retaliation for the recent drone and missile attack on the Jewish state.
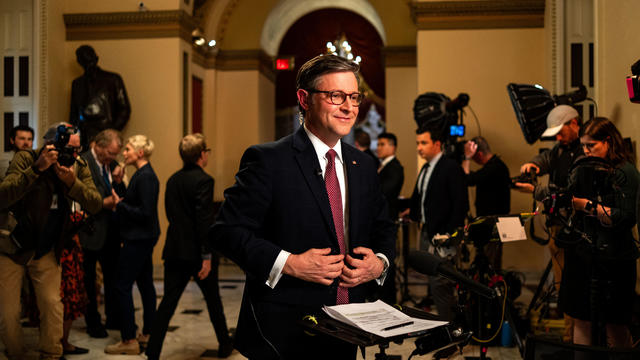
Democrats may have to offer Johnson a lifeline if it comes to a vote, given Republicans' razor-thin majority.

Trump Media & Technology Group sent a letter to Nasdaq warning that so-called "naked" short selling could be impacting its stock.

Maxwell Anderson, 33, has been charged with first-degree intentional homicide in the death of 19-year-old Sade Robinson.

Fans are furiously dissecting the lyrics of "The Tortured Poets Department," with some speculating the tracks are about Joe Alwyn, Matty Healy, Travis Kelce and Kim Kardashian.

The singer was found deceased at her home, a representative said.

North Korea's latest launch to boost Kim Jong Un's image wasn't a missile, but a song and music video all about the "Friendly Father."

Caretaker Jessy Kurczewski says her friend mixed vodka and Visine for a buzz.

There are 20 missing persons cases and 36 unsolved homicides listed on the cards.

A disappearing lizard population in the mountains of Arizona shows how climate change is fast-tracking the rate of extinction.

Eliminating player "proposition" bets may be one way to discourage athletes from betting on sports, experts said.
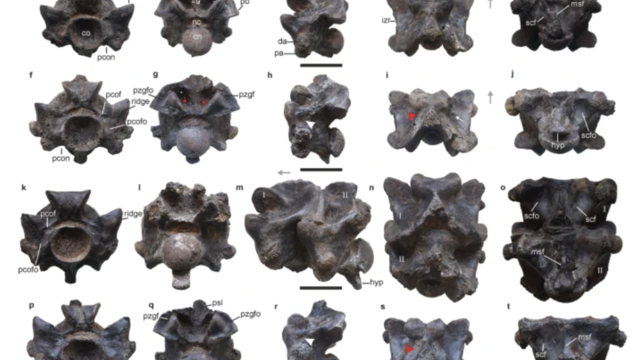
The Vasuki indicus specimen dates back 47 million years and is more than double the average size of similar snakes, like pythons.

Direct conflict between Israel and Iran, which threaten global oil supplies and could drive up energy costs, has investors on edge.

Starbucks unveiled the new cups ahead of Earth Day and as a new report warns plastic production emissions are even greater than those from aviation.

The soprano recounted an anecdote from the book's foreword by Francis Collins, which describes an impromptu sing-along at a dinner party attended by Supreme Court justices.

The MY 2024 Cybertrucks have faulty accelerator pedals that may be dislodged when high force is applied, the company said.

Twelve people have been selected to serve as jurors in former President Donald Trump's criminal trial in New York, filling out the panel on the third day of proceedings.

Under the 5th Amendment, the jury is prohibited from holding it against former President Donald Trump if he does not testify.

The jurors are tasked with deciding the outcome of the first criminal trial of a former president in U.S. history.

They backed the president even as their brother makes his own bid for Biden's job.

It came with Europe bracing for the possibility of a second Trump term.

The allies want the leaders to reconnect ahead of another potential Trump term, sources confirm.

The Treasury Department announced sanctions on two entities accused of fundraising for extremist West Bank settlers.

Rep. Ilhan Omar's daughter says she was one of three students suspended from Barnard College.

After Israel accused the U.N. of failing to "do its job," the head of a U.N. aid agency said it's Israel that's delaying the flow.

With gold prices teetering on the edge of $2,400, here's how you can find the best price available now.

Borrowing your home equity could lead to savings compared to other options. Find out how much you'd save here.

A drop in home sales could prove to be an opportunity for some buyers. Here's why.

CEO Mark Zuckerberg's newest AI-powered Meta AI agents started venturing into social media this week to engage with real people.

Eliminating player "proposition" bets may be one way to discourage athletes from betting on sports, experts said.

Retailers are ditching and limiting shelf-checkout at some stores, particularly those hit by theft and customer complaints.

Trump Media & Technology Group sent a letter to Nasdaq warning that so-called "naked" short selling could be impacting its stock.

Direct conflict between Israel and Iran, which threaten global oil supplies and could drive up energy costs, has investors on edge.

From Hey Dude shoes to a luxury toilet upgrade, Sam's Club shoppers are going wild for these trending products.

These luggage pieces from Rimowa, Away, Monos and more are made to last a lifetime. Here's where to buy them now.

Stave off unsightly wrinkles and keep garments sanitary with the best clothes steamers on the market.

The full jury and one alternate have been selected in Donald Trump's "hush money" trial in New York. Five more alternate jurors are needed. The judge has said opening statements could start Monday. Attorney and CBS News campaign reporter Katrina Kaufman has more.

CBS News' data analysis found 425 bridges in 36 states over waterways used by large vessels had inadequate pier protection.

President Biden warned about risking a wider war in the Middle East, and while the White House is monitoring the situation, there has been no official response. National Security Advisor Jake Sullivan met virtually Thursday with Israeli leaders, but it is unclear if Israel told U.S. leaders about the planned strike on Iran.

A JetBlue flight from Washington to Boston began to take off at the same time a Southwest jet was crossing the same runway. Both planes stopped moments before a potential collision.

Actor Marcia Gay Harden sits down with Seth Doane to discuss her CBS series "So Help Me Todd," her LGBTQ+ activism and her love of pottery. Then, Jonathan Vigliotti meets Julian Curi, the filmmaker behind the short film "Gruff." "Here Comes the Sun" is a closer look at some of the people, places and things we bring you every week on "CBS Sunday Morning."

Comedian and actor Kevin James sits down with Jim Axelrod to discuss his Amazon Prime special "Kevin James: Irregardless,” and the journey he has taken throughout his career. Then, Robert Costa visits the National Gallery of Art in Washington, D.C., to view an exhibit on artist Mark Rothko’s work. “Here Comes the Sun” is a closer look at some of the people, places and things we bring you every week on “CBS Sunday Morning.”

Actor Paul Giamatti sits down with Lesley Stahl to discuss his latest film, “The Holdovers,” as well as other characters he has portrayed throughout his career. Then, Seth Doane travels to the Musée d’Orsay in Paris to learn about the AI-generated avatar of Vincent Van Gogh. “Here Comes the Sun” is a closer look at some of the people, places and things we bring you every week on “CBS Sunday Morning.”

Actor Hilary Swank sits down with Tracy Smith to discuss her latest film, “Ordinary Angels.” Then, Conor Knighton travels to New Orleans to meet portraitist Michael Deas and to learn about his paintings found on stamps, Time magazine covers and more. “Here Comes the Sun” is a closer look at some of the people, places and things we bring you every week on “CBS Sunday Morning.”

Actor Charles Melton sits down with Tracy Smith to discuss his latest film, “May December.” Then, Conor Knighton travels to Las Vegas to attend The World of Concrete’s annual convention. “Here Comes the Sun” is a closer look at some of the people, places and things we bring you every week on “CBS Sunday Morning.”

The singer was found deceased at her home, a representative said.

Starbucks unveiled the new cups ahead of Earth Day and as a new report warns plastic production emissions are even greater than those from aviation.

Renée Fleming is a five-time Grammy winner, a Kennedy Center honoree and a longtime advocate for the healing power of the arts. For her new book "Music and Mind," Fleming collected essays from leading scientists, artists and health care providers. They look at the powerful impact that music and the arts can have on our health.

"E! News" co-host Keltie Knight is revealing details about her private battle with a chronic health condition in hopes of helping others. The Emmy Award winner revealed last month that she was having a hysterectomy to treat a chronic and severe form of anemia. She spoke candidly about the decision on Instagram.

It’s a new era for Taylor Swift and her fans. The superstar dropped her new album “The Tortured Poets Department.” She then surprised fans with an additional 15 tracks.

In New York, we tour a unique museum that’s home to an extensive collection of toys, games and playgrounds. Then, we sit down with NBA superstar Steph Curry to discuss his heartwarming new children’s book. Watch these stories and more on "Eye on America" with host Michelle Miller.

In Arizona, we learn why flag football is becoming an increasingly popular sport, especially among girls. Then in New York, we meet with descendants of some of the most notable suffragists of the 20th century. Watch these stories and more on "Eye on America" with host Michelle Miller.

In Connecticut, we meet the preservationists who are giving dilapidated lighthouses new life. Then in California, we learn about the efforts to restore an iconic fishing boat. Watch these stories and more on "Eye on America" with host Michelle Miller.

In Louisiana, we learn how a devastating drought has greatly diminished the area’s crawfish supply. Then in Ohio, we tour a small business that’s seeing promising results from a four-day work week model. Watch these stories and more on Eye on America with host Michelle Miller.
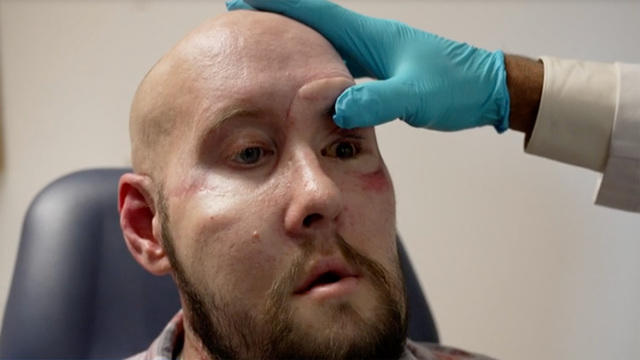
In New York, we speak with the patient and medical team behind the first successful eye transplant. Then in Arizona, we get a firsthand look at a breathing technique that proponents claim can create a healing psychedelic state without any drugs. Watch these stories and more on "Eye on America" with host Michelle Miller.

Spencer, the official mascot of the Boston Marathon, is honored by his community. David Begnaud introduces us to a woman who calls herself a "bad weather friend" – because she's there when you need her most. Plus, more heartwarming stories.

Russ Cook says the scariest part of his run through Africa was "on the back of a motorbike, thinking I was about to die."

A trendsetting third grader creates a school tradition to don dapper outfits on Wednesdays. A retiree makes it her mission to thank those who may be in thankless jobs. Plus, more heartwarming and inspiring stories.

Lyn Story is a retiree whose mission is to be the "bad weather friend," someone who is there for you in a time of need. David Begnaud shows how her huge heart led to life-changing friendships.

Nets star Mikal Bridges fulfills his dream of teaching by working at a school in Brooklyn for the day. A doctor overcomes the odds to help other survivors of catastrophic injuries. Plus, behind the scenes of Drew Barrymore's talk show, and more heartwarming stories.

CBS Reports goes to Illinois, which has one of the highest rates of institutionalization in the country, to understand the challenges families face keeping their developmentally disabled loved ones at home.

As more states legalize gambling, online sportsbooks have spent billions courting the next generation of bettors. And now, as mobile apps offer 24/7 access to placing wagers, addiction groups say more young people are seeking help than ever before. CBS Reports explores what experts say is a hidden epidemic lurking behind a sports betting bonanza that's leaving a trail of broken lives.

In February 2023, a quiet community in Ohio was blindsided by disaster when a train derailed and authorities decided to unleash a plume of toxic smoke in an attempt to avoid an explosion. Days later, residents and the media thought the story was over, but in fact it was just beginning. What unfolded in East Palestine is a cautionary tale for every town and city in America.

In the aftermath of the Supreme Court striking down affirmative action in college admissions, CBS Reports examines the fog of uncertainty for students and administrators who say the decision threatens to unravel decades of progress.

CBS Reports examines the legacy of the U.S. government's terrorist watchlist, 20 years after its inception. In the years since 9/11, the database has grown exponentially to target an estimated 2 million people, while those who believe they were wrongfully added are struggling to clear their names.

The CDC estimates the U.S. could reach 300 measles cases this year.

A person self-immolated at a park across from the courthouse where former President Donald Trump's New York criminal trial is taking place.

The singer was found deceased at her home, a representative said.
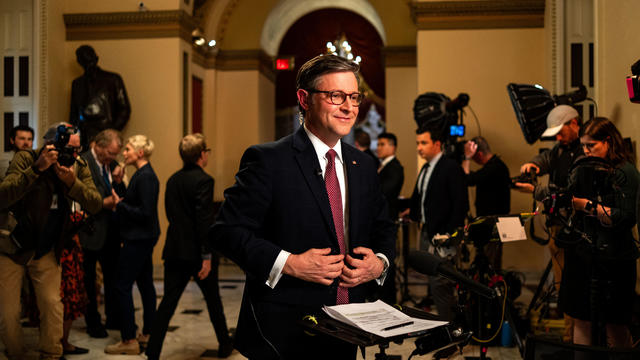
Democrats may have to offer Johnson a lifeline if it comes to a vote, given Republicans' razor-thin majority.

Fans are furiously dissecting the lyrics of "The Tortured Poets Department," with some speculating the tracks are about Joe Alwyn, Matty Healy, Travis Kelce and Kim Kardashian.

Retailers are ditching and limiting shelf-checkout at some stores, particularly those hit by theft and customer complaints.

Eliminating player "proposition" bets may be one way to discourage athletes from betting on sports, experts said.

Trump Media & Technology Group sent a letter to Nasdaq warning that so-called "naked" short selling could be impacting its stock.

The Treasury Department announced sanctions on two entities accused of fundraising for extremist West Bank settlers connected to violence against Palestinians.

The MY 2024 Cybertrucks have faulty accelerator pedals that may be dislodged when high force is applied, the company said.

A person self-immolated at a park across from the courthouse where former President Donald Trump's New York criminal trial is taking place.
Democrats may have to offer Johnson a lifeline if it comes to a vote, given Republicans' razor-thin majority.

The Treasury Department announced sanctions on two entities accused of fundraising for extremist West Bank settlers connected to violence against Palestinians.

The final five alternate jurors in former President Donald Trump's New York criminal trial were selected on Friday.

The bills are part of a complicated plan by Speaker Mike Johnson to get badly needed lethal aid to Ukraine, as well as security funding for Israel and Taiwan.

The CDC estimates the U.S. could reach 300 measles cases this year.

Health officials are warning consumers not to consume Infinite Herbs basil sold at some Trader Joe's and Dierberg's stores after 12 people were sickened.

A landmark review for Britain's National Health Service found young people have been let down by "remarkably weak" evidence backing medical interventions in gender care.

Organic option is best when buying certain produce, especially blueberries, nonprofit group says in analysis of chemical residues.

British lawmakers have backed legislation that would see the legal age to buy tobacco increase by one year every year until it's eventually banned.

North Korea's latest launch to boost Kim Jong Un's image wasn't a missile, but a song and music video all about the "Friendly Father."

The Treasury Department announced sanctions on two entities accused of fundraising for extremist West Bank settlers connected to violence against Palestinians.

The break in tradition does not sit well with the Association of Summer Olympic Committee, who said it undermines "the value of Olympism and the uniqueness of the games."

The Vasuki indicus specimen dates back 47 million years and is more than double the average size of similar snakes, like pythons.

Paris police cordoned off an area around an Iranian consulate amid reports of a man threatening to detonate a bomb, but a suspect was quickly detained.

The singer was found deceased at her home, a representative said.

The soprano recounted an anecdote from the book's foreword by Francis Collins, which describes an impromptu sing-along at a dinner party attended by Supreme Court justices.

Fans are furiously dissecting the lyrics of "The Tortured Poets Department," with some speculating the tracks are about Joe Alwyn, Matty Healy, Travis Kelce and Kim Kardashian.

Renée Fleming is a five-time Grammy winner, a Kennedy Center honoree and a longtime advocate for the healing power of the arts. For her new book "Music and Mind," Fleming collected essays from leading scientists, artists and health care providers. They look at the powerful impact that music and the arts can have on our health.

"E! News" co-host Keltie Knight is revealing details about her private battle with a chronic health condition in hopes of helping others. The Emmy Award winner revealed last month that she was having a hysterectomy to treat a chronic and severe form of anemia. She spoke candidly about the decision on Instagram.

A bipartisan group of lawmakers has introduced a bill supporting the development of nuclear fusion power. Hank Jenkins-Smith, professor of public policy at the University of Oklahoma, joins CBS News to discuss.

Sen. Maria Cantwell is backing an amended bill that could lead to a ban of TikTok in the U.S.

From labor shortages to environmental impacts, farmers are looking to AI to help revolutionize the agriculture industry. One California startup, Farm-ng, is tapping into the power of AI and robotics to perform a wide range of tasks, including seeding, weeding and harvesting.

U.S. Senators are pressing banks to take more actions to help victims of wire fraud. CBS News national consumer investigative correspondent Anna Werner has more on how Americans are being scammed.

Artificial intelligence has become so advanced it has now surpassed human performance in several basic tasks, according to a new report from Stanford University's Institute for Human-Centered Artificial Intelligence. Russell Wald, deputy director of the institute, joins CBS News to unpack more key findings from the study.

Starbucks unveiled the new cups ahead of Earth Day and as a new report warns plastic production emissions are even greater than those from aviation.

A report from the United Nations determined that 1 million species are threatened with extinction. Dr. John Wiens from the University of Arizona believes that number is far higher based on his research. He says climate change is quickening the threat of extinction for species, including a 3-million-year-old lizard population previously found in the Arizona mountains.

A disappearing lizard population in the mountains of Arizona shows how climate change is fast-tracking the rate of extinction.

Some of the most critically endangered birds on the planet have been released back into the wild. CBS News national environmental correspondent David Schechter has more on the harsh conditions Puerto Rican parrots face, and the people working to save them.

Scientists are using a range of tools to protect the endangered wildlife that could disappear in coming decades.

Caretaker Jessy Kurczewski says her friend mixed vodka and Visine for a buzz.

There are 20 missing persons cases and 36 unsolved homicides listed on the cards.

The final five alternate jurors in former President Donald Trump's New York criminal trial were selected on Friday.

Maxwell Anderson, 33, has been charged with first-degree intentional homicide in the death of 19-year-old Sade Robinson.

Dennis Dechaine is serving a life sentence for the murder and sexual assault of Sarah Cherry, who disappeared while babysitting in 1988.

NASA confirmed Monday that a mystery object that crashed through the roof of a Naples, Florida home last month was space junk from equipment discarded by the space station.

NASA said it agrees with an independent review board that concluded the project could cost up to $11 billion without major changes.

It was a "bittersweet moment" as United Launch Alliance brought the Delta program to a close.

NASA flight engineers managed to photograph and videotape the moon's shadow on Earth about 260 miles below them.

Millions of Americans poured into the solar eclipse’s path of totality to watch in wonder. The excitement was shared across generations for the rare celestial event that saw watch parties across the country as almost all of the continental U.S. saw at least a partial solar eclipse.

A look back at the esteemed personalities who've left us this year, who'd touched us with their innovation, creativity and humanity.

The Francis Scott Key Bridge in Baltimore collapsed early Tuesday, March 26 after a column was struck by a container ship that reportedly lost power, sending vehicles and people into the Patapsco River.

When Tiffiney Crawford was found dead inside her van, authorities believed she might have taken her own life. But could she shoot herself twice in the head with her non-dominant hand?

We look back at the life and career of the longtime host of "Sunday Morning," and "one of the most enduring and most endearing" people in broadcasting.

Cayley Mandadi's mother and stepfather go to extreme lengths to prove her death was no accident.

The final alternate jurors have been seated in former President Donald Trump's criminal "hush money" trial. Opening statements in the trial are set to begin Monday. CBS News campaign reporter Katrina Kaufman is following the latest, and CBS News legal contributor Jessica Levinson breaks down how the case could play out.

Saturday marks 25 years since the devastating Columbine High School shooting in Littleton, Colorado. Twelve students and one teacher were killed when a pair of students opened fire during a school day in what became one of the most high-profile mass shootings in American history. Dave Cullen, author of the book "Columbine," joined CBS News to discuss that tragic day.

At midnight Friday, Taylor Swift released her highly anticipated album, "The Tortured Poets Department," and two hours later she surprised fans with 15 additional songs as part of the "Anthology" version of the album. "Entertainment Tonight" correspondent Denny Directo joined CBS News to talk about the new music.
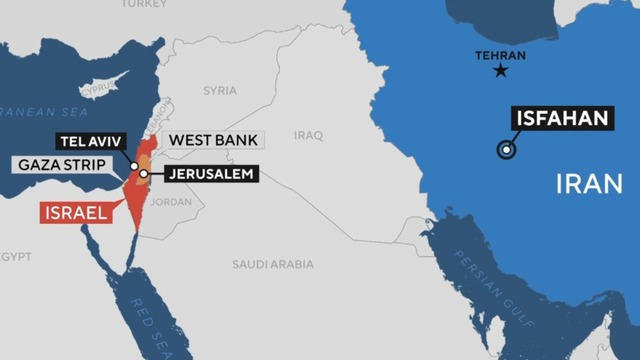
U.S. officials have told CBS News that Israel attacked Iran early Friday and Iran's state-run media is reporting that three drones were shot down over the central city of Isfahan, which houses sites associated with the country's nuclear program. Israel's allies, including the U.S., have warned against any action that could further raise tensions in the region. Dan Raviv, co-author of "Spies Against Armageddon: Inside Israel's Secret Wars," joined CBS News to discuss the strike.
Just before midnight Thursday, the House advanced several stand-alone measures on foreign aid and U.S. border security thanks to the support of four Democrats, but the bills may cost Speaker Mike Johnson his job. CBS News congressional correspondent Nikole Killion has more.