
Pope Francis says "a negotiated peace is better than a war without end"
In an exclusive interview with CBS News' Norah O'Donnell, Pope Francis called for "negotiated peace" in Ukraine and Gaza, noting the devastating effects war has on children.
Watch CBS News

In an exclusive interview with CBS News' Norah O'Donnell, Pope Francis called for "negotiated peace" in Ukraine and Gaza, noting the devastating effects war has on children.

An Arizona grand jury indicted 18 people in connection with an alleged attempt to use alternate electors after the 2020 election.

"It's a good day for America, it's a good day for Europe and it's a good day for world peace," Mr. Biden said in remarks from the White House.

Earlier this month, the Arizona Supreme Court ruled that the highly-restrictive 160-year-old law that bans nearly all abortions can be enforced.

Two sources briefed on the situation told CBS News the agent spouted gibberish, was speaking incoherently and provoked another officer physically.

House Speaker Mike Johnson was met with loud boos as he visited Columbia University, where he joined calls for the president's resignation amid pro-Palestinian protests.

CDC's provisional figures show a 2% decline in births from 2022 to 2023.

Campus Department of Public Safety officers visited the encampment, instructed students not to hang signs, flags or other materials from trees and posts in the park, and warned them not to use megaphones.

Classes at James Bowie High School were canceled for Thursday.

The Supreme Court heard arguments in a case that pits Idaho's near-total abortion ban against a federal law that requires hospitals to offer emergency care.

Cal Poly Humboldt will remain closed through at least the weekend after pro-Palestinian protesters clashed with police, and demonstrators occupied buildings and refused to leave.
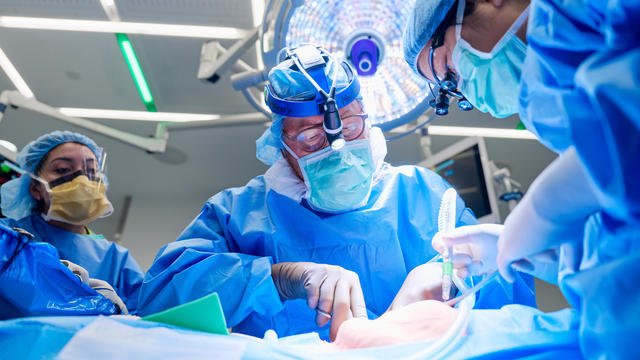
For the first time, surgeons at NYU Langone Health performed a combined mechanical heart pump and gene-edited pig kidney transplant into a living person.

Ann Mayers entered AurGroup Credit Union on April 19 and "demanded money while displaying a handgun," police said.

Paul Grice, 31, was arrested and charged by Oklahoma authorities with murder and kidnapping in connection to the deaths of Veronica Butler and Jilian Kelley.

Two-year-old Tyler Fabregas asked his mother "Where's Beyoncé?" in a viral TikTok video she posted last week from Manila.

This 2024 "State of the Air" report warns efforts to reduce emissions are undermined by extreme heat, drought and wildfires caused by climate change.

Gustav Klimt's "Portrait of Fräulein Lieser," which went missing after its owners fled Austria after 1930, was auctioned off for $32 million.

Federal officials say they're double checking whether pasteurization has eradicated the danger from possible bird virus particles in milk.

There are no cameras allowed in the court where Trump is being tried on 34 felony counts stemming from a "hush money" payment before the 2016 election.

Jurors in former President Donald Trump's trial in New York heard testimony from a former media executive about his efforts to bury negative stories about Trump before the 2016 presidential election.

Trump made 10 social media posts that were "threatening, inflammatory," prosecutors said, arguing he should pay a fine for each post.

The FBI calls on tech companies to "step up" to protect people looking for love online.

Niselio Barros Garcia Jr., 50, scammed victims out of $2.3 million in funds, according to authorities.

Scammers have been increasingly successful in leveraging their romantic grip on victims.

Summer Lee has defeated Bhavini Patel in the Democratic primary for Pennsylvania's 12th Congressional District, the Associated Press projects.

He could receive a large windfall from his newly public media company, Trump Media & Technology Group.

Protesters have been arrested at Columbia and Yale as they've called for a break from Israel.
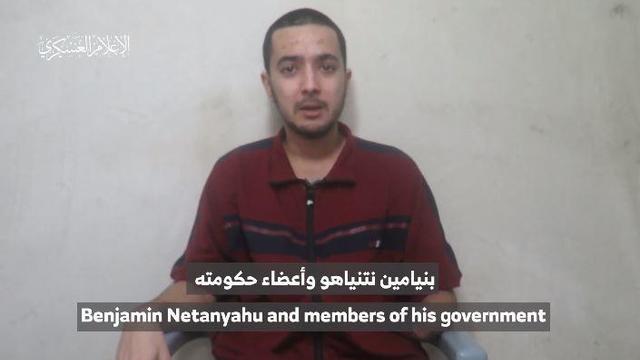
The video appears to show U.S.-Israeli hostage Hersh Goldberg-Polin delivering a message under duress.

Columbia University has given students 48 hours to dismantle their pro-Palestinian protest on the school's main lawn.

The Netzah Yehuda Battalion of the Israel Defense Forces has faced criticism for its conduct. Will the U.S. take action?

If you're thinking about getting a home equity loan, you may want to do so before May. Here's why.

A debt relief service may be able to help you deal with mounting debt. Here's why now is a great time to sign up.

There are a few reasons why you may want to put some money in gold before the Fed meets again. Here's what to know.

Trump Media CEO Devin Nunes is asking four House committees to investigate possible "naked" short selling in the company's shares.

Expanded federal overtime rule could result in employers paying workers an additional $1.5 billion, according to one estimate.

Travelers often spend more than they need to for airfare, experts say. Here's what to know about paying for add-ons like your seat assignment.

Lawmakers argue the Chinese government can use the widely popular video-sharing app as a spy tool and to covertly influence the U.S. public.

Regulators prohibit new noncompetes, which impede millions of U.S. workers from getting a better job.

Receive a $40 Digital Costco Shop Card when you join as a new member at Costco.com when entering PARA24 at checkout.

These best cooling floor fans from Dyson, Honeywell, Black+Decker and more will cool you in the months ahead.

The best meal kits for weight loss make it easy (and fun!) to stick to a healthy, consistent diet.

Pope Francis called for countries at war to negotiate in an exclusive interview with "CBS Evening News" anchor and managing editor Norah O'Donnell in Rome. "A negotiated peace is better than a war without end," the pontiff said. "Look to negotiate. Look for peace."

"CBS Evening News" anchor and managing editor Norah O'Donnell was given a private tour of the magnificent St. Peter's Basilica, the largest church in the world, located in the smallest nation in the world.
The Supreme Court on Wednesday listened to arguments over whether Idaho's near-total abortion ban violates a federal law that requires hospitals that participate in Medicare to provide necessary stabilizing treatment, including emergency abortion care. Jan Crawford reports.

Arizona's House of Representatives on Wednesday advanced an effort to repeal the state's Civil War-era abortion ban that's set to go into effect June 8. CBS News campaign reporter Shawna Mizelle has the latest from Phoenix.

Pope Francis called for countries at war to negotiate in an exclusive interview with "CBS Evening News" anchor and managing editor Norah O'Donnell in Rome. "A negotiated peace is better than a war without end," the pontiff said. "Look to negotiate. Look for peace."

CBS News asked Catholics in cities across the U.S. about their relationship with the church and how they feel about the pope. Nikki Battiste has more.

The Supreme Court on Wednesday listened to arguments over whether Idaho's near-total abortion ban violates a federal law that requires hospitals that participate in Medicare to provide necessary stabilizing treatment, including emergency abortion care. Jan Crawford reports.
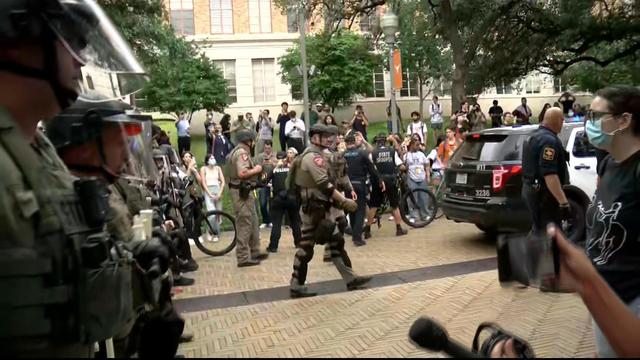
Pro-Palestinian demonstrations are taking place at universities across the U.S., including in California, Texas and New York. Wednesday marked the eighth day of a contentious protest at Columbia University that prompted the school to cancel in-person classes and brought a visit from House Speaker Mike Johnson. Nancy Chen has the latest.

"CBS Evening News" anchor and managing editor Norah O'Donnell was given a private tour of the magnificent St. Peter's Basilica, the largest church in the world, located in the smallest nation in the world.

President Biden and his reelection campaign clearly state they need Latino support this November. However, several polls in recent months have revealed an increasing number of Latino voters preferring former President Donald Trump. CBS News political director Fin Gómez and Democratic strategist Chuck Rocha join to discuss more.

"CBS Evening News" anchor and managing editor Norah O'Donnell was given a private tour of the magnificent St. Peter's Basilica, the largest church in the world, located in the smallest nation in the world.

CBS News asked Catholics in cities across the U.S. about their relationship with the church and how they feel about the pope. Nikki Battiste has more.

In an exclusive interview with CBS News' Norah O'Donnell, Pope Francis called for "negotiated peace" in Ukraine and Gaza, noting the devastating effects war has on children.

Two-year-old Tyler Fabregas asked his mother "Where's Beyoncé?" in a viral TikTok video she posted last week from Manila.

All this week, CBS News has been investigating online romance scams. In this final installment, Jim Axelrod looks at what law enforcement and lawmakers can do -- but also why it's important for the online dating industry to police itself.

When President Biden signed a foreign aid bill Wednesday that includes tens of billions of dollars in assistance to Ukraine, Israel and Taiwan, it was touted as money that would "strengthen our national security and send a message to the world about the power of American leadership." Retired Lt. Gen. H.R. McMaster, former national security adviser, joins CBS News with analysis.

The Transportation Department announced new rules Wednesday requiring airlines to issue automatic cash refunds for flight cancelations or delays, delayed baggage returns and services like Wi-Fi or seat selection that are paid for but not provided. Transportation Secretary Pete Buttigieg joins CBS News to discuss the changes and how airlines are reacting.

American schools are facing layoffs as enrollment falls and pandemic-era aid dries up. CBS News reporter Bo Erickson has the details.

Testimony is expected to resume Thursday in former President Donald Trump's New York criminal trial. CBS News legal analyst Rikki Klieman joins with more.

At his lowest moment, U.S. Army veteran and former teacher Billy Keenan found strength in his faith as he was reminded of his own resilience.

A surfing accident left New York teacher Billy Keenan paralyzed, but when he received a call from a police officer, his life changed.

The So Much To Give Inclusive Cafe in Cedars, Pennsylvania employs 63 people — 80% have a disability.

A mom was worried about what her son, who has autism, would do after high school. So she opened the So Much To Give cafe, a restaurant in Cedars, Pennsylvania, that employs people with disabilities – and helps them grow.

David Begnaud visits Jeffrey Olsen, known as the "Toy Man" in Vista, California, who has dedicated over 30 years to donating toys, food, and clothes to those in need.

CBS Reports goes to Illinois, which has one of the highest rates of institutionalization in the country, to understand the challenges families face keeping their developmentally disabled loved ones at home.

As more states legalize gambling, online sportsbooks have spent billions courting the next generation of bettors. And now, as mobile apps offer 24/7 access to placing wagers, addiction groups say more young people are seeking help than ever before. CBS Reports explores what experts say is a hidden epidemic lurking behind a sports betting bonanza that's leaving a trail of broken lives.

In February 2023, a quiet community in Ohio was blindsided by disaster when a train derailed and authorities decided to unleash a plume of toxic smoke in an attempt to avoid an explosion. Days later, residents and the media thought the story was over, but in fact it was just beginning. What unfolded in East Palestine is a cautionary tale for every town and city in America.

In the aftermath of the Supreme Court striking down affirmative action in college admissions, CBS Reports examines the fog of uncertainty for students and administrators who say the decision threatens to unravel decades of progress.

CBS Reports examines the legacy of the U.S. government's terrorist watchlist, 20 years after its inception. In the years since 9/11, the database has grown exponentially to target an estimated 2 million people, while those who believe they were wrongfully added are struggling to clear their names.

CDC's provisional figures show a 2% decline in births from 2022 to 2023.

An Arizona grand jury indicted 18 people in connection with an alleged attempt to use alternate electors after the 2020 election.

Two sources briefed on the situation told CBS News the agent spouted gibberish, was speaking incoherently and provoked another officer physically.

Paul Grice, 31, was arrested and charged by Oklahoma authorities with murder and kidnapping in connection to the deaths of Veronica Butler and Jilian Kelley.

Two-year-old Tyler Fabregas asked his mother "Where's Beyoncé?" in a viral TikTok video she posted last week from Manila.

Proponents say a sweeping ban on noncompete clauses should boost workers, but the new rules face serious legal challenges.

Egg prices are jumping as an outbreak of highly pathogenic avian influenza forces producers to slaughter millions of infected birds.

New Transportation Department rules could save consumers $500 million annually, Transportation Secretary Pete Buttigieg said.

Niselio Barros Garcia Jr., 50, scammed victims out of $2.3 million in funds, according to authorities.

Trump Media CEO Devin Nunes is asking four House committees to investigate possible "naked" short selling in the company's shares.

An Arizona grand jury indicted 18 people in connection with an alleged attempt to use alternate electors after the 2020 election.

Two sources briefed on the situation told CBS News the agent spouted gibberish, was speaking incoherently and provoked another officer physically.

Four-year-old Abigail Mor Edan was held by Hamas for 50 days and was the youngest American hostage released by Hamas.

House Speaker Mike Johnson was met with loud boos as he visited Columbia University, where he joined calls for the president's resignation amid pro-Palestinian protests.

The New Jersey Democrat suffered "a cardiac episode based on complications from his diabetes" earlier this month, his office said.

CDC's provisional figures show a 2% decline in births from 2022 to 2023.
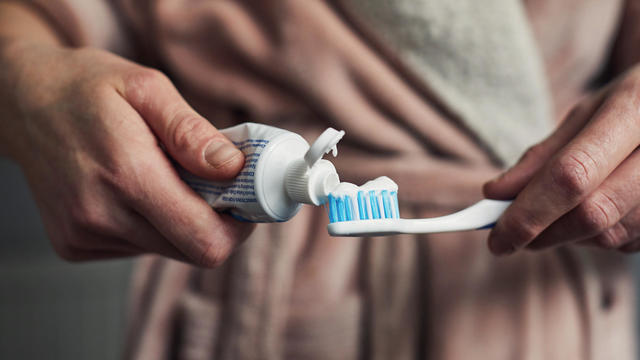
Don't brush your teeth after breakfast? Or after vomiting? Dentists say it can wear away your enamel. Here's what to do instead.

Federal officials say they're double checking whether pasteurization has eradicated the danger from possible bird virus particles in milk.

For the first time, surgeons at NYU Langone Health performed a combined mechanical heart pump and gene-edited pig kidney transplant into a living person.

The USDA had floated banning flavored milk options from some school lunches.

In an exclusive interview with CBS News' Norah O'Donnell, Pope Francis called for "negotiated peace" in Ukraine and Gaza, noting the devastating effects war has on children.

Two-year-old Tyler Fabregas asked his mother "Where's Beyoncé?" in a viral TikTok video she posted last week from Manila.

Four-year-old Abigail Mor Edan was held by Hamas for 50 days and was the youngest American hostage released by Hamas.

Gustav Klimt's "Portrait of Fräulein Lieser," which went missing after its owners fled Austria after 1930, was auctioned off for $32 million.

A video released by Hamas' military wing appears to show U.S.-Israeli hostage Hersh Goldberg-Polin delivering a message under duress.

Two-year-old Tyler Fabregas asked his mother "Where's Beyoncé?" in a viral TikTok video she posted last week from Manila.

Country music star Blake Shelton expands his popular bar and music venue 'Ole Red' from Nashville to Las Vegas. This opening coincides with Shelton stepping back from his prominent TV roles.

Surprise guests, a broken foot and a history-making headliner.

Eric Church is revered as one of country music's most respected figures, often described as Nashville's renegade. But he admits that even after his success, he sometimes still sees himself as an outsider.

Angel Carter Conrad talks about her brother Aaron Carter, his death and how she hopes his legacy and previously unheard music can help others.

Lawmakers argue the Chinese government can use the widely popular video-sharing app as a spy tool and to covertly influence the U.S. public.

NASA's Voyager 1, the first spacecraft to travel beyond our solar system, has started sending information back to Earth again after scientists managed to fix the probe from 15 billion miles away.

From labor shortages to environmental impacts, farmers are looking to AI to help revolutionize the agriculture industry. One California startup, Farm-ng, is tapping into the power of AI and robotics to perform a wide range of tasks, including seeding, weeding and harvesting.

Customers who rely on government assistance programs can get same perks as Prime members, for less.

Secretary of Commerce Gina Raimondo is at the center of a global competition for semiconductor dominance. It's a battle that also puts her at the center of two of the hottest global national security hotspots. Lesley Stahl of 60 Minutes spoke with Raimondo for the broadcast.

Emerging cicadas are so loud in one South Carolina county that residents are calling the sheriff's office asking why they can hear a "noise in the air that sounds like a siren, or a whine, or a roar." CBS News' John Dickerson has details.

Representatives from across the world are gathering in Ottawa, Canada, to negotiate a potential treaty to limit plastic pollution. CBS News national environmental correspondent David Schechter has the latest on the talks.

"Although to some, the noise is annoying, they pose no danger to humans or pets," the sheriff wrote. "Unfortunately, it is the sounds of nature."

The White House is considering declaring a national climate emergency to unlock federal powers and stifle oil development, according to a Bloomberg report. Meanwhile, the Biden administration is announcing several projects this Earth Week. Columbia University Climate School professor Dr. Melissa Lott joins with analysis.

NASA's Voyager 1, the first spacecraft to travel beyond our solar system, has started sending information back to Earth again after scientists managed to fix the probe from 15 billion miles away.

All this week, CBS News has been investigating online romance scams. In this final installment, Jim Axelrod looks at what law enforcement and lawmakers can do -- but also why it's important for the online dating industry to police itself.

Paul Grice, 31, was arrested and charged by Oklahoma authorities with murder and kidnapping in connection to the deaths of Veronica Butler and Jilian Kelley.

Ann Mayers entered AurGroup Credit Union on April 19 and "demanded money while displaying a handgun," police said.

Niselio Barros Garcia Jr., 50, scammed victims out of $2.3 million in funds, according to authorities.

Glenn Sullivan Sr., 54, pleaded guilty to four counts of second-degree rape on April 17.

In November 2023, NASA's Voyager 1 spacecraft stopped sending "readable science and engineering data."

In two weeks, Boeing's Starliner spacecraft is scheduled to launch its first piloted test flight, bringing two veteran NASA astronauts to the International Space Station. Astronaut Matt Dominick joined CBS News from the ISS to talk about the mission and life in space.

A process called cryopreservation allows cells to remain frozen but alive for hundreds of years. For some animal cells, the moon is the closest place that's cold enough.

The Lyrid meteor show is set to peak as the week begins.

April's full moon, known as the Pink Moon, will reach peak illumination on Tuesday, but it will appear full from Monday morning through Thursday morning.

A look back at the esteemed personalities who've left us this year, who'd touched us with their innovation, creativity and humanity.

The Francis Scott Key Bridge in Baltimore collapsed early Tuesday, March 26 after a column was struck by a container ship that reportedly lost power, sending vehicles and people into the Patapsco River.

When Tiffiney Crawford was found dead inside her van, authorities believed she might have taken her own life. But could she shoot herself twice in the head with her non-dominant hand?

We look back at the life and career of the longtime host of "Sunday Morning," and "one of the most enduring and most endearing" people in broadcasting.

Cayley Mandadi's mother and stepfather go to extreme lengths to prove her death was no accident.

Emerging cicadas are so loud in one South Carolina county that residents are calling the sheriff's office asking why they can hear a "noise in the air that sounds like a siren, or a whine, or a roar." CBS News' John Dickerson has details.

All this week, CBS News has been investigating online romance scams. In this final installment, Jim Axelrod looks at what law enforcement and lawmakers can do -- but also why it's important for the online dating industry to police itself.

When President Biden signed a foreign aid bill Wednesday that includes tens of billions of dollars in assistance to Ukraine, Israel and Taiwan, it was touted as money that would "strengthen our national security and send a message to the world about the power of American leadership." Retired Lt. Gen. H.R. McMaster, former national security adviser, joins CBS News with analysis.

The Transportation Department announced new rules Wednesday requiring airlines to issue automatic cash refunds for flight cancelations or delays, delayed baggage returns and services like Wi-Fi or seat selection that are paid for but not provided. Transportation Secretary Pete Buttigieg joins CBS News to discuss the changes and how airlines are reacting.

American schools are facing layoffs as enrollment falls and pandemic-era aid dries up. CBS News reporter Bo Erickson has the details.