
Protests over Israel-Hamas war lead to hundreds of arrests on campus
Hundreds of people have been arrested in California, New York, Massachusetts, Texas and other states during the tense protests on college campuses.
Watch CBS News

Hundreds of people have been arrested in California, New York, Massachusetts, Texas and other states during the tense protests on college campuses.

The Supreme Court convened to consider whether former President Donald Trump is entitled to broad immunity from criminal charges in the 2020 election case.

Harvey Weinstein's 2020 conviction on felony sex crime charges has been overturned by the State of New York Court of Appeals.

Follow live updates of Donald Trump's New York criminal trial, where former National Enquirer boss David Pecker is testifying for the third day.

A former high school athletic director was arrested Thursday morning after allegedly using artificial intelligence to impersonate the school principal in a recording that included racist and antisemitic comments.

A federal judge has denied former President Donald Trump's request for a new trial in the civil suit brought by the writer E. Jean Carroll, who was awarded an $83.3 million judgment.

The petitions are the latest in the effort for Ryan Corbett's release.

President Joe Biden has signed legislation that could lead to TikTok being sold or banned. Here's who might buy it — and for how much.

U.S. regulators are reviving a rescinded rule, laying the groundwork for for a major court fight with the broadband industry.
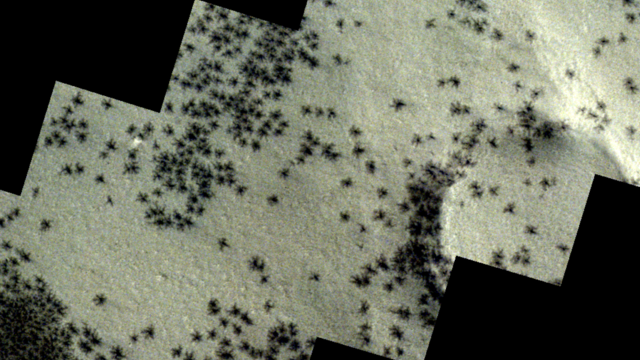
The creepy patterns were observed by the European Space Agency's ExoMars Trace Gas Orbiter.

David Schultz's wife said that the person found was wearing boots that matched her husband's, and his keys were found in the pants pocket.

A cross unearthed in eastern Poland likely belonged to an outcasted Russian religious community around 300 years ago.

Looking for a place to live in NYC? Zillow is now listing Frank Sinatra and Mia Farrow's former home on the Upper East Side.

A photo of the raft the man is believed to have used shows just a few long planks assembled together.

The Shenzhou 18 crew will replace three taikonauts aboard the Chinese space station who are wrapping up a six-month stay.

The renowned Moulin Rouge cabaret venue's director has vowed to "rise to the challenge" after the windmill's sails fell off.

A mass stranding of long-finned pilot whales in Western Australia led to the deaths of 29 of the creatures that beached near a tourist town.

Taylor Swift fans have found a way to feel "a little bit closer to" their hero at a London watering hole, and The Black Dog pub is lapping it up.

There are no cameras allowed in the court where Trump is being tried on 34 felony counts stemming from a "hush money" payment before the 2016 election.

Jurors in former President Donald Trump's trial in New York heard testimony from a former media executive about his efforts to bury negative stories about Trump before the 2016 presidential election.

Trump made 10 social media posts that were "threatening, inflammatory," prosecutors said, arguing he should pay a fine for each post.

The FBI calls on tech companies to "step up" to protect people looking for love online.

Laura Kowal's match on an online dating site wasn't what he seemed. Now her daughter is on a mission to expose the risk of romance scams: "It could happen to anybody."

Scammers have been increasingly successful in leveraging their romantic grip on victims.

Summer Lee has defeated Bhavini Patel in the Democratic primary for Pennsylvania's 12th Congressional District, the Associated Press projects.

He could receive a large windfall from his newly public media company, Trump Media & Technology Group.

Protesters have been arrested at Columbia and Yale as they've called for a break from Israel.

As Israel's leader equates U.S. university protests to rallies in Nazi Germany, Palestinian students tell CBS News what the support means to them.

House Speaker Mike Johnson was met with loud boos as he visited Columbia University, where he joined calls for the president's resignation amid pro-Palestinian protests.
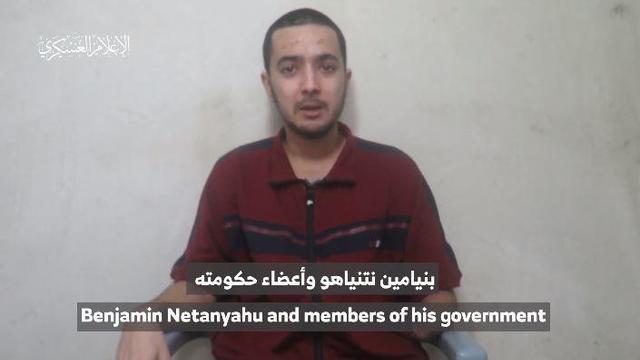
The video appears to show U.S.-Israeli hostage Hersh Goldberg-Polin delivering a message under duress.

Do you have $7,500 or more in credit card debt? Here are a few ways to pay it off quickly.

Looking to make a successful investment in gold? Then be sure to avoid making these simple mistakes.

You don't have to accept a low interest rate on your savings. There are many great account options to consider.

Visitors will have to pay five euros, a fee designed to offset some of the costs of accommodating tourists.

President Joe Biden has signed legislation that could lead to TikTok being sold or banned. Here's who might buy it — and for how much.

These are the airports Southwest is pulling out of completely as it looks to save costs.

Only one vehicle of the 10 small SUVs tested earned a good rating.

Real GDP increased at an annual rate of 1.6% in the first quarter of 2024, according to initial estimate.

Receive a $40 Digital Costco Shop Card when you join as a new member at Costco.com when entering PARA24 at checkout.

Wondering if Medicare covers hearing aids? Learn more about which plans offer coverage for for hearing aids.

Find that special someone by signing up for one of the undeniably best dating apps in 2024.

A New York appeals court overturned Harvey Weinstein's 2020 conviction on felony sex crimes. The court ruled that the disgraced movie mogul did not have a fair trial because the judge who presided over the case allowed women to testify about allegations that were not part of the charges against him. Weinstein will remain in prison because of his rape conviction in Los Angeles.

Former President Donald Trump's lawyers are in for a long day with the Supreme Court hearing Trump's immunity claim in Washington, D.C., and testimony resuming in his "hush money" case in New York. CBS News' Rob Legare and Errol Barnett have the latest on the two cases. And CBS News legal analyst Rikki Klieman has a breakdown of the New York case.

Another tense day of protests over the Israel-Hamas war is expected on college campuses across the country on Thursday. Hundreds of people have already been arrested since the demonstrations began. CBS News Boston reporter Penny Kmitt reports.

Jerry Seinfeld and Jim Gaffigan reunite in the new movie "Unfrosted," directed by Seinfeld. The film humorously depicts the 1963 race between cereal giants Kellogg's and Post to invent the first breakfast pastry, featuring Seinfeld as a fictional Kellogg's executive and Gaffigan as the CEO.

In this episode of "Person to Person with Norah O’Donnell," O’Donnell speaks with CVS Health CEO and author Karen Lynch about her life and career.

In this episode of Person to Person with Norah O’Donnell, O’Donnell speaks with author and professor Adam Grant about his newest book, as he discusses unlocking your hidden potential.

In this episode of Person to Person with Norah O’Donnell, O’Donnell speaks with author and professor Arthur Brooks about his partnership with Oprah Winfrey and the key to living a happier life.

In this episode of Person to Person with Norah O’Donnell, O’Donnell speaks with Senator Mitt Romney about his place in the Republican party, his family’s influence and what’s next for him in politics.

In this episode of Person to Person with Norah O’Donnell, O’Donnell speaks with Dolly Parton about her new book on her costumes and clothing and her new rock album.

In an exclusive interview with "CBS Evening News" anchor and managing editor Norah O’Donnell, Pope Francis discusses the wars in Ukraine and Gaza and calls for negotiating peace.

President Biden and his reelection campaign clearly state they need Latino support this November. However, several polls in recent months have revealed an increasing number of Latino voters preferring former President Donald Trump. CBS News political director Fin Gómez and Democratic strategist Chuck Rocha join to discuss more.

"CBS Evening News" anchor and managing editor Norah O'Donnell was given a private tour of the magnificent St. Peter's Basilica, the largest church in the world, located in the smallest nation in the world.

CBS News asked Catholics in cities across the U.S. about their relationship with the church and how they feel about the pope. Nikki Battiste has more.

In an exclusive interview with CBS News' Norah O'Donnell, Pope Francis called for "negotiated peace" in Ukraine and Gaza, noting the devastating effects war has on children.

In California, we dine out at a restaurant powered by robots. Then in Washington, we take a sip of a beanless cup of coffee, which aims to reduce the environmental impact of the popular beverage. Watch these stories and more on "Eye on America" with host Michelle Miller.

In New York, we tour a unique museum that’s home to an extensive collection of toys, games and playgrounds. Then, we sit down with NBA superstar Steph Curry to discuss his heartwarming new children’s book. Watch these stories and more on "Eye on America" with host Michelle Miller.

In Arizona, we learn why flag football is becoming an increasingly popular sport, especially among girls. Then in New York, we meet with descendants of some of the most notable suffragists of the 20th century. Watch these stories and more on "Eye on America" with host Michelle Miller.

In Connecticut, we meet the preservationists who are giving dilapidated lighthouses new life. Then in California, we learn about the efforts to restore an iconic fishing boat. Watch these stories and more on "Eye on America" with host Michelle Miller.

In Louisiana, we learn how a devastating drought has greatly diminished the area’s crawfish supply. Then in Ohio, we tour a small business that’s seeing promising results from a four-day work week model. Watch these stories and more on Eye on America with host Michelle Miller.

At his lowest moment, U.S. Army veteran and former teacher Billy Keenan found strength in his faith as he was reminded of his own resilience.

A surfing accident left New York teacher Billy Keenan paralyzed, but when he received a call from a police officer, his life changed.

The So Much To Give Inclusive Cafe in Cedars, Pennsylvania employs 63 people — 80% have a disability.

A mom was worried about what her son, who has autism, would do after high school. So she opened the So Much To Give cafe, a restaurant in Cedars, Pennsylvania, that employs people with disabilities – and helps them grow.

David Begnaud visits Jeffrey Olsen, known as the "Toy Man" in Vista, California, who has dedicated over 30 years to donating toys, food, and clothes to those in need.

CBS Reports goes to Illinois, which has one of the highest rates of institutionalization in the country, to understand the challenges families face keeping their developmentally disabled loved ones at home.

As more states legalize gambling, online sportsbooks have spent billions courting the next generation of bettors. And now, as mobile apps offer 24/7 access to placing wagers, addiction groups say more young people are seeking help than ever before. CBS Reports explores what experts say is a hidden epidemic lurking behind a sports betting bonanza that's leaving a trail of broken lives.

In February 2023, a quiet community in Ohio was blindsided by disaster when a train derailed and authorities decided to unleash a plume of toxic smoke in an attempt to avoid an explosion. Days later, residents and the media thought the story was over, but in fact it was just beginning. What unfolded in East Palestine is a cautionary tale for every town and city in America.

In the aftermath of the Supreme Court striking down affirmative action in college admissions, CBS Reports examines the fog of uncertainty for students and administrators who say the decision threatens to unravel decades of progress.

CBS Reports examines the legacy of the U.S. government's terrorist watchlist, 20 years after its inception. In the years since 9/11, the database has grown exponentially to target an estimated 2 million people, while those who believe they were wrongfully added are struggling to clear their names.

U.S. regulators are reviving a rescinded rule, laying the groundwork for for a major court fight with the broadband industry.

Follow live updates of Donald Trump's New York criminal trial, where former National Enquirer boss David Pecker is testifying for the third day.

Visitors will have to pay five euros, a fee designed to offset some of the costs of accommodating tourists.

Hundreds of people have been arrested in California, New York, Massachusetts, Texas and other states during the tense protests on college campuses.

PayPal payments are being made to 117,044 consumers whose videos may have been accessed by unauthorized users.

U.S. regulators are reviving a rescinded rule, laying the groundwork for for a major court fight with the broadband industry.

Visitors will have to pay five euros, a fee designed to offset some of the costs of accommodating tourists.

PayPal payments are being made to 117,044 consumers whose videos may have been accessed by unauthorized users.

President Joe Biden has signed legislation that could lead to TikTok being sold or banned. Here's who might buy it — and for how much.

These are the airports Southwest is pulling out of completely as it looks to save costs.

Follow live updates of Donald Trump's New York criminal trial, where former National Enquirer boss David Pecker is testifying for the third day.

The petitions are the latest in the effort for Ryan Corbett's release.

A federal judge has denied former President Donald Trump's request for a new trial in the civil suit brought by the writer E. Jean Carroll, who was awarded an $83.3 million judgment.

Coal-fired power plants would have to capture smokestack emissions or shut down under a new EPA rule the industry says would make the grid less reliable. It's likely to face court challenges.

The Supreme Court convened to consider whether former President Donald Trump is entitled to broad immunity from criminal charges in the 2020 election case.

CDC's provisional figures show a 2% decline in births from 2022 to 2023.
Don't brush your teeth after breakfast? Or after vomiting? Dentists say it can wear away your enamel. Here's what to do instead.

Federal officials say they're double checking whether pasteurization has eradicated the danger from possible bird virus particles in milk.
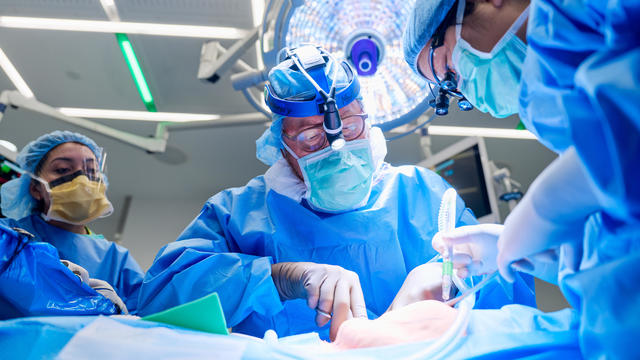
For the first time, surgeons at NYU Langone Health performed a combined mechanical heart pump and gene-edited pig kidney transplant into a living person.

The USDA had floated banning flavored milk options from some school lunches.

The petitions are the latest in the effort for Ryan Corbett's release.

A cross unearthed in eastern Poland likely belonged to an outcasted Russian religious community around 300 years ago.

Hundreds of people have been arrested in California, New York, Massachusetts, Texas and other states during the tense protests on college campuses.

The creepy patterns were observed by the European Space Agency's ExoMars Trace Gas Orbiter.

Italy's Culture Ministry has banned loans of works to the Minneapolis Institute of Art, following a dispute with the U.S. museum over an ancient marble statue believed to have been looted from Italy almost a half-century ago.

Looking for a place to live in NYC? Zillow is now listing Frank Sinatra and Mia Farrow's former home on the Upper East Side.

Italy's Culture Ministry has banned loans of works to the Minneapolis Institute of Art, following a dispute with the U.S. museum over an ancient marble statue believed to have been looted from Italy almost a half-century ago.

The renowned Moulin Rouge cabaret venue's director has vowed to "rise to the challenge" after the windmill's sails fell off.

Taylor Swift fans have found a way to feel "a little bit closer to" their hero at a London watering hole, and The Black Dog pub is lapping it up.

Jerry Seinfeld and Jim Gaffigan reunite in the new movie "Unfrosted," directed by Seinfeld. The film humorously depicts the 1963 race between cereal giants Kellogg's and Post to invent the first breakfast pastry, featuring Seinfeld as a fictional Kellogg's executive and Gaffigan as the CEO.

U.S. regulators are reviving a rescinded rule, laying the groundwork for for a major court fight with the broadband industry.

Meta began rolling out its new AI-powered smart assistant software, saying it will be integrated across Instagram, Facebook and Messenger. Adam Auriemma, editor-in-chief for CNET, joined CBS News to discuss the new tool.

From labor shortages to environmental impacts, farmers are looking to AI to help revolutionize the agriculture industry. One California startup, Farm-ng, is tapping into the power of AI and robotics to perform a wide range of tasks, including seeding, weeding and harvesting.

Lawmakers argue the Chinese government can use the widely popular video-sharing app as a spy tool and to covertly influence the U.S. public.

NASA's Voyager 1, the first spacecraft to travel beyond our solar system, has started sending information back to Earth again after scientists managed to fix the probe from 15 billion miles away.

Emerging cicadas are so loud in one South Carolina county that residents are calling the sheriff's office asking why they can hear a "noise in the air that sounds like a siren, or a whine, or a roar." CBS News' John Dickerson has details.

Representatives from across the world are gathering in Ottawa, Canada, to negotiate a potential treaty to limit plastic pollution. CBS News national environmental correspondent David Schechter has the latest on the talks.

"Although to some, the noise is annoying, they pose no danger to humans or pets," the sheriff wrote. "Unfortunately, it is the sounds of nature."

The White House is considering declaring a national climate emergency to unlock federal powers and stifle oil development, according to a Bloomberg report. Meanwhile, the Biden administration is announcing several projects this Earth Week. Columbia University Climate School professor Dr. Melissa Lott joins with analysis.

NASA's Voyager 1, the first spacecraft to travel beyond our solar system, has started sending information back to Earth again after scientists managed to fix the probe from 15 billion miles away.

A New York appeals court overturned Harvey Weinstein's 2020 conviction on felony sex crimes. The court ruled that the disgraced movie mogul did not have a fair trial because the judge who presided over the case allowed women to testify about allegations that were not part of the charges against him. Weinstein will remain in prison because of his rape conviction in Los Angeles.

Harvey Weinstein's 2020 conviction on felony sex crime charges has been overturned by the State of New York Court of Appeals.

William Ray Grimes was indicted on charges of murder and burglary in the 2012 slaying of Lowell Badger, police said.

All this week, CBS News has been investigating online romance scams. In this final installment, Jim Axelrod looks at what law enforcement and lawmakers can do -- but also why it's important for the online dating industry to police itself.

Paul Grice, 31, was arrested and charged by Oklahoma authorities with murder and kidnapping in connection to the deaths of Veronica Butler and Jilian Kelley.

The creepy patterns were observed by the European Space Agency's ExoMars Trace Gas Orbiter.

The Shenzhou 18 crew will replace three taikonauts aboard the Chinese space station who are wrapping up a six-month stay.

In November 2023, NASA's Voyager 1 spacecraft stopped sending "readable science and engineering data."

In two weeks, Boeing's Starliner spacecraft is scheduled to launch its first piloted test flight, bringing two veteran NASA astronauts to the International Space Station. Astronaut Matt Dominick joined CBS News from the ISS to talk about the mission and life in space.

A process called cryopreservation allows cells to remain frozen but alive for hundreds of years. For some animal cells, the moon is the closest place that's cold enough.

A look back at the esteemed personalities who've left us this year, who'd touched us with their innovation, creativity and humanity.

The Francis Scott Key Bridge in Baltimore collapsed early Tuesday, March 26 after a column was struck by a container ship that reportedly lost power, sending vehicles and people into the Patapsco River.

When Tiffiney Crawford was found dead inside her van, authorities believed she might have taken her own life. But could she shoot herself twice in the head with her non-dominant hand?

We look back at the life and career of the longtime host of "Sunday Morning," and "one of the most enduring and most endearing" people in broadcasting.

Cayley Mandadi's mother and stepfather go to extreme lengths to prove her death was no accident.

The Supreme Court has concluded arguments over Donald Trump's claim he is entitled to broad immunity from federal prosecution for allegedly official acts while he was in the White House. Nancy Cordes anchored CBS News' special report on the arguments.

The Supreme Court heard arguments Thursday in Trump v. United States, a case weighing whether former President Donald Trump should be immune from federal prosecution for his actions while serving in the White House. CBS News' Jessica Levinson, Jan Crawford and Scott MacFarlane break down the historic arguments that played out in court.

A fourth temporary channel is opening for the Port of Baltimore one month after the Francis Scott Key Bridge collapsed. Two victims of the collapse still have not been recovered as crews continue to remove the wreckage. Col. Estee Pinchasin, Baltimore District commander for the U.S. Army Corps of Engineers, joined CBS News to discuss the recovery.

Lisa Guerrera is the founder of New York City-based skincare beauty startup Experiment. She joined CBS News to talk about how TikTok has impacted her business and what a nationwide ban would mean for her and other entrepreneurs and content creators who rely on the platform.

Former White House chief of staff Mark Meadows and former New York City Mayor Rudy Giuliani are among the 18 people who have been charged in Arizona for an alleged fake electors scheme to try to overturn the 2020 election. Although some of the defendants' names, including Meadows and Giuliani, were redacted from the court documents, they were identified based on the descriptions. CBS News election law contributor David Becker has more on the case.